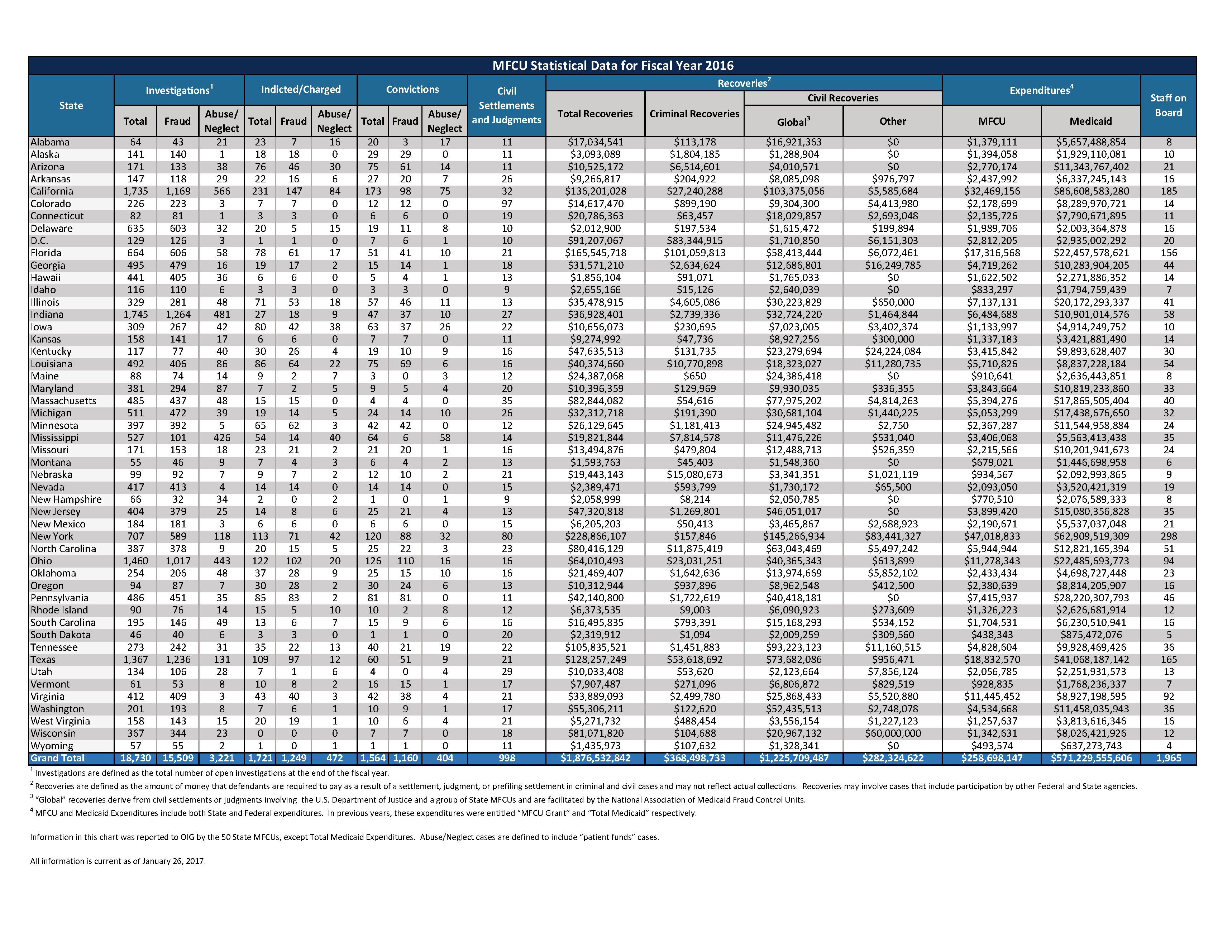
Florida has proved to be one of the most effective states in the nation last year for recovering Medicaid fraud money.
A report issued by the U.S. Department of Health and Human Services revealed Florida recovered more than $165 million in otherwise lost funds through fraudulent Medicaid cases during fiscal year 2015-2016, the state’s attorney general said in a statement Thursday.
The report shows Attorney General Pam Bondi’s Medicaid Fraud Control Unit (MFCU) is working, according to the Office of Inspector General for Health and Human Services.
“My Medicaid Fraud Control Unit investigators work tirelessly to stop Medicaid fraud and recover stolen funds for taxpayers,” Bondi said in the statement. “This report sends the strong message that we will continue to aggressively pursue anyone trying to defraud Florida’s Medicaid program.”
According to the report, Florida ranked only second in the nation in total funds recovered for the 2015-2016 fiscal year, with New York raking in the most at nearly $229,000,000.
Since taking office in 2011, Bondi’s MFCU has obtained more than half a billion dollars in settlements and judgments in total.
The unit investigates and prosecutes providers that intentionally defraud the state’s Medicaid program through fraudulent billing practices. In addition, the MFCU investigates allegations of patient abuse, neglect and exploitation in facilities receiving payments under the Medicaid program.
Each year OIG of the HHS publishes a report of the Medicaid Fraud Control Unit statistical data from the preceding federal fiscal year.
California and Texas ranked third and fourth, respectively, with California saving more than $136,000,000 and Texas saving more than $128,000,000.
To view HHS OIG’s report, click here.